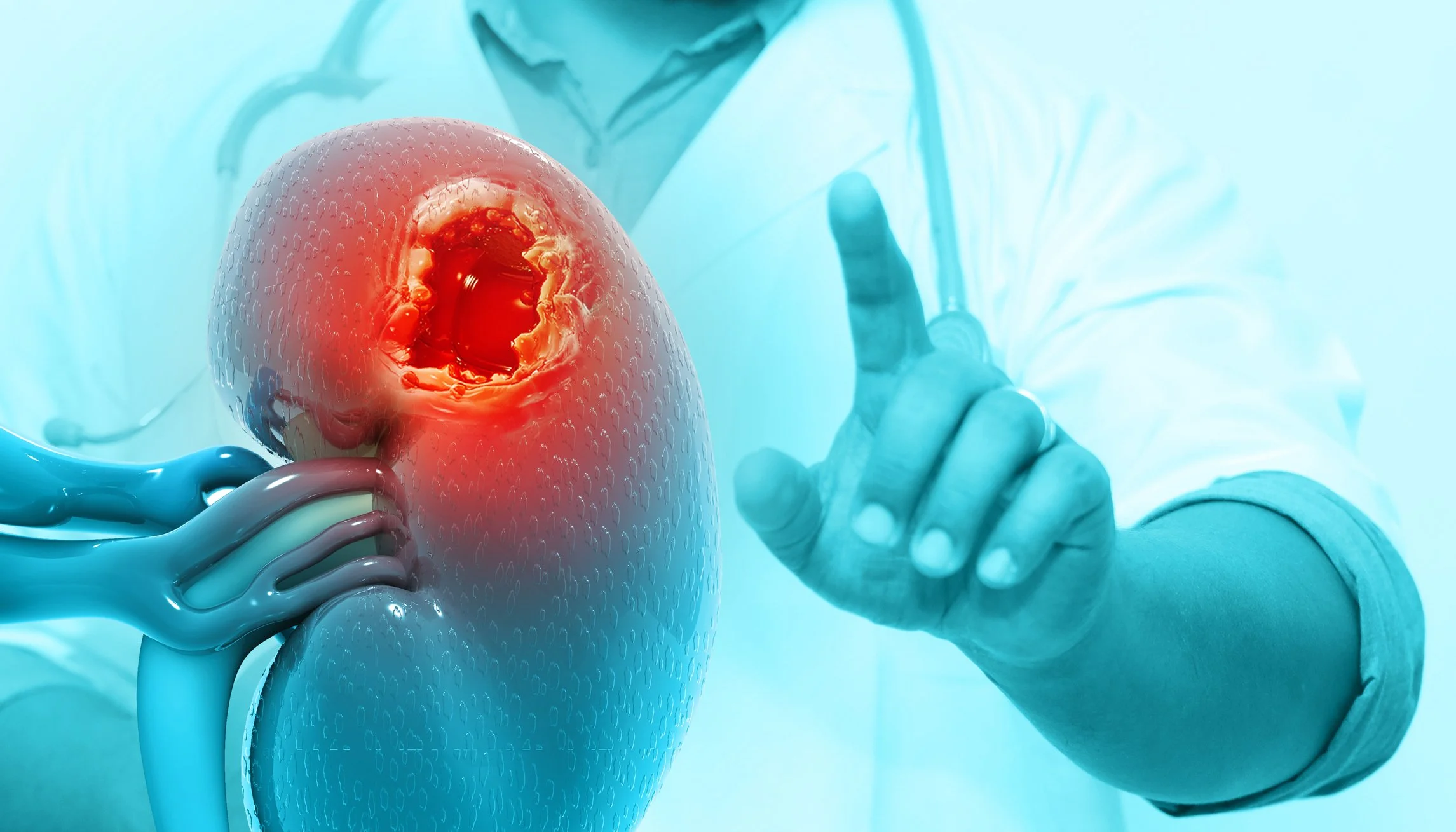
Kidney Mass Found Incidentally: What the Workup Involves
Most kidney masses are not found because of symptoms. They are found because someone had a scan for something else — back pain, a bowel check, a vague abdominal ache — and the radiologist noted a lesion on the kidney that wasn't the reason for the scan at all.
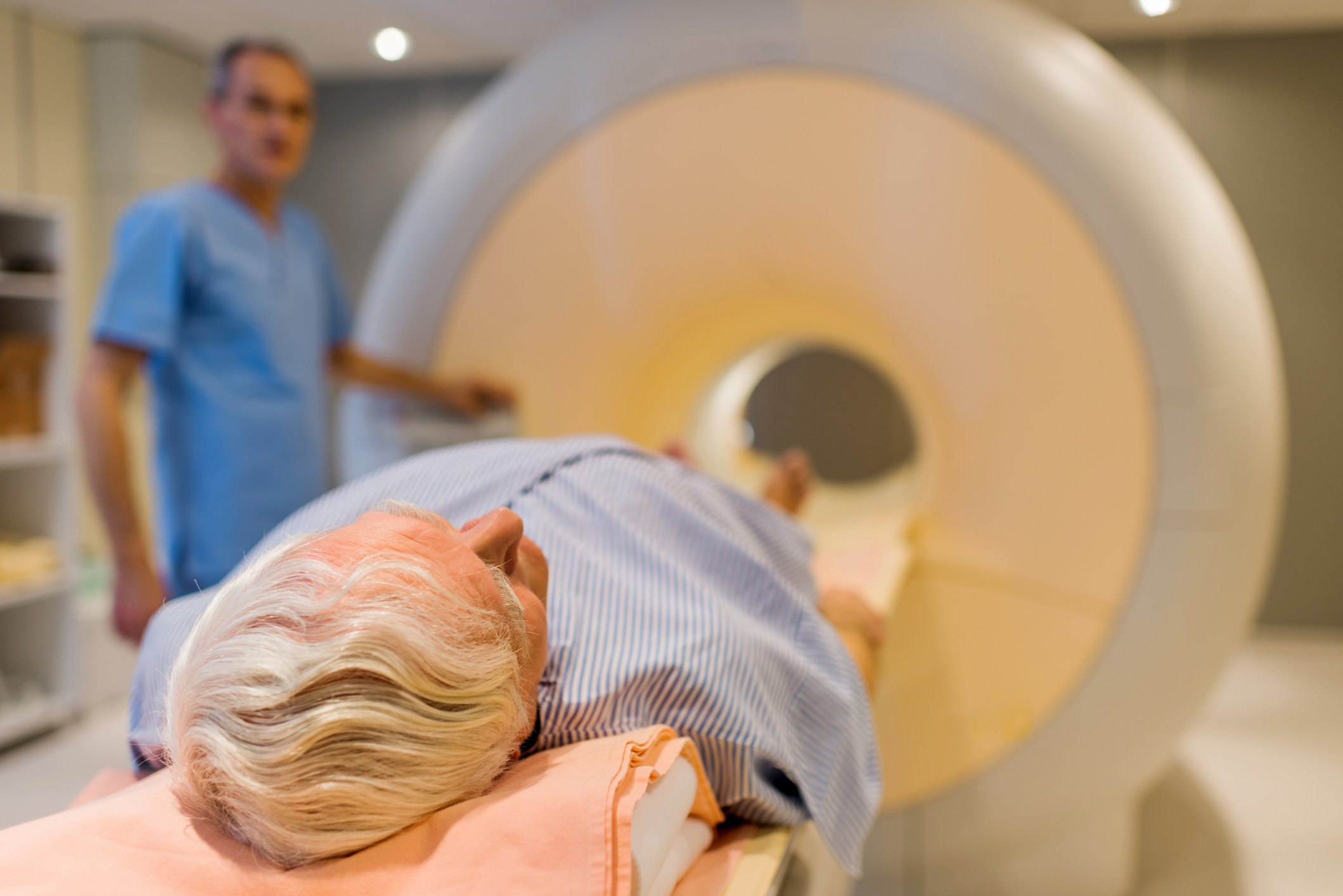
MRI of the Prostate: What It Shows and What Happens Next
If your GP has referred you for a prostate MRI, or your urologist has recommended one after an elevated PSA, you are probably wondering what the scan actually shows — and more importantly, what it means if something is found.
This article explains what a prostate MRI involves, how results are reported, and how the findings guide the next steps. The goal is to make the process less opaque before you go in.

Blood in Urine: When Is It Cancer and What Happens Next?
Noticing blood in your urine is frightening. It is the kind of symptom that stops people mid-thought and sends them straight to their phone to search for answers, usually late at night when they are already worried.
This article explains what blood in the urine actually means, when it needs urgent attention, and what a proper assessment involves. The goal is to replace anxiety with information — so that whatever is causing it, you know what to do next.

High-Risk Prostate Cancer: Is Surgery Still an Option?
Most prostate cancer content focuses on low and intermediate risk disease — the slow-growing cancers, the active surveillance conversations, the "you have time to decide" reassurances. That is reasonable, because most prostate cancers detected today fall into those categories.
But some don't. And the patients sitting across the desk with high-risk disease are often the ones who feel most unsupported by what they find online.
This article is for them.

Red Flags in Primary Care: When to Refer for Suspected Urological Cancer
The urological cancers most likely to present through general practice — prostate, kidney and bladder — are often detectable at a stage where treatment options are meaningful. The referrals that matter most are the ones where a GP recognises a red flag early and moves on it.
This guide focuses on the cancer-relevant triggers that warrant urological assessment, what to include, and when to move urgently.
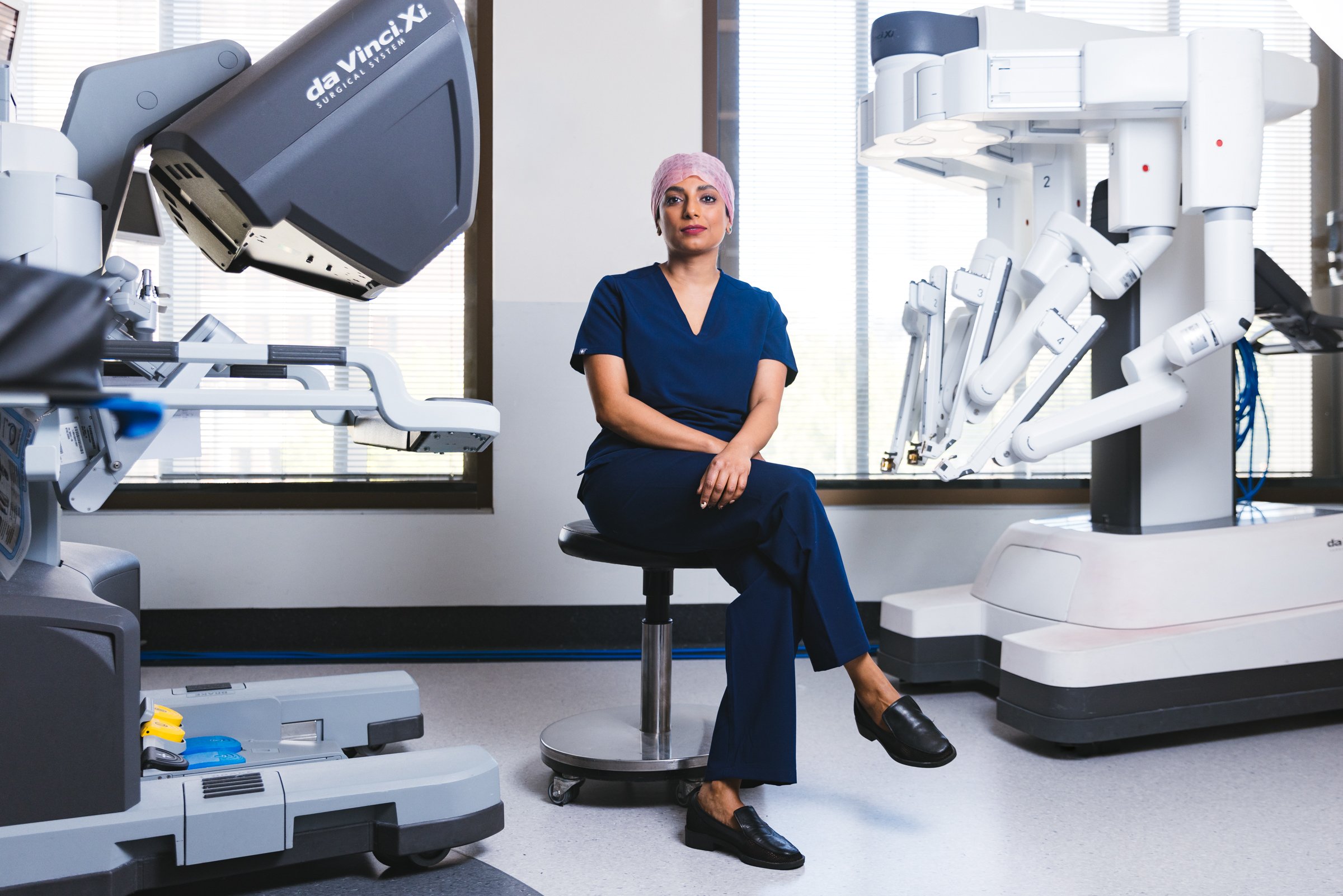
Robotic Surgery Training: What It Involves and What Patients Should Ask
When patients research robotic surgery, they focus almost entirely on the technology. The da Vinci system. The four arms. The magnified 3D view. What the robot can and can't do.
What they focus on less — but what matters more — is the surgeon operating it.
Robotic surgery is a platform. Like any surgical platform, its value depends almost entirely on the person using it: their technical training, their judgement about when to use it and when not to, and their ability to handle the unexpected when it arises mid-operation.
This article explains what serious training in robotic urologic cancer surgery actually looks like, and what questions are worth asking before you commit to a surgeon.

Nerve-Sparing Prostatectomy: When It's Safe, When It Isn't, and How the Decision Is Made
The questions most people bring into a prostate cancer surgery consultation aren't always the ones they say out loud. Will I be incontinent? Will I be able to have erections? If you try to spare the nerves, are you going to leave cancer behind?
These are the right questions. They sit at the heart of one of the most consequential decisions in prostate cancer surgery — whether to attempt nerve-sparing, to what extent, and on which side.
This article explains what nerve-sparing involves, what it can and cannot achieve, and how I approach the decision with patients when the answer isn't straightforward. Because often, it isn't.
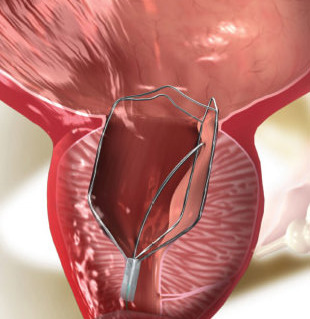
iTind for Enlarged Prostate (BPH): What to Expect, Who It Suits, and How It Compares
Thinking about iTind for BPH and wondering what it’s actually like? This practical guide walks through the 5–7 days the device is in place, common temporary symptoms, activity restrictions, what happens on removal day, and how recovery typically unfolds over the following weeks.
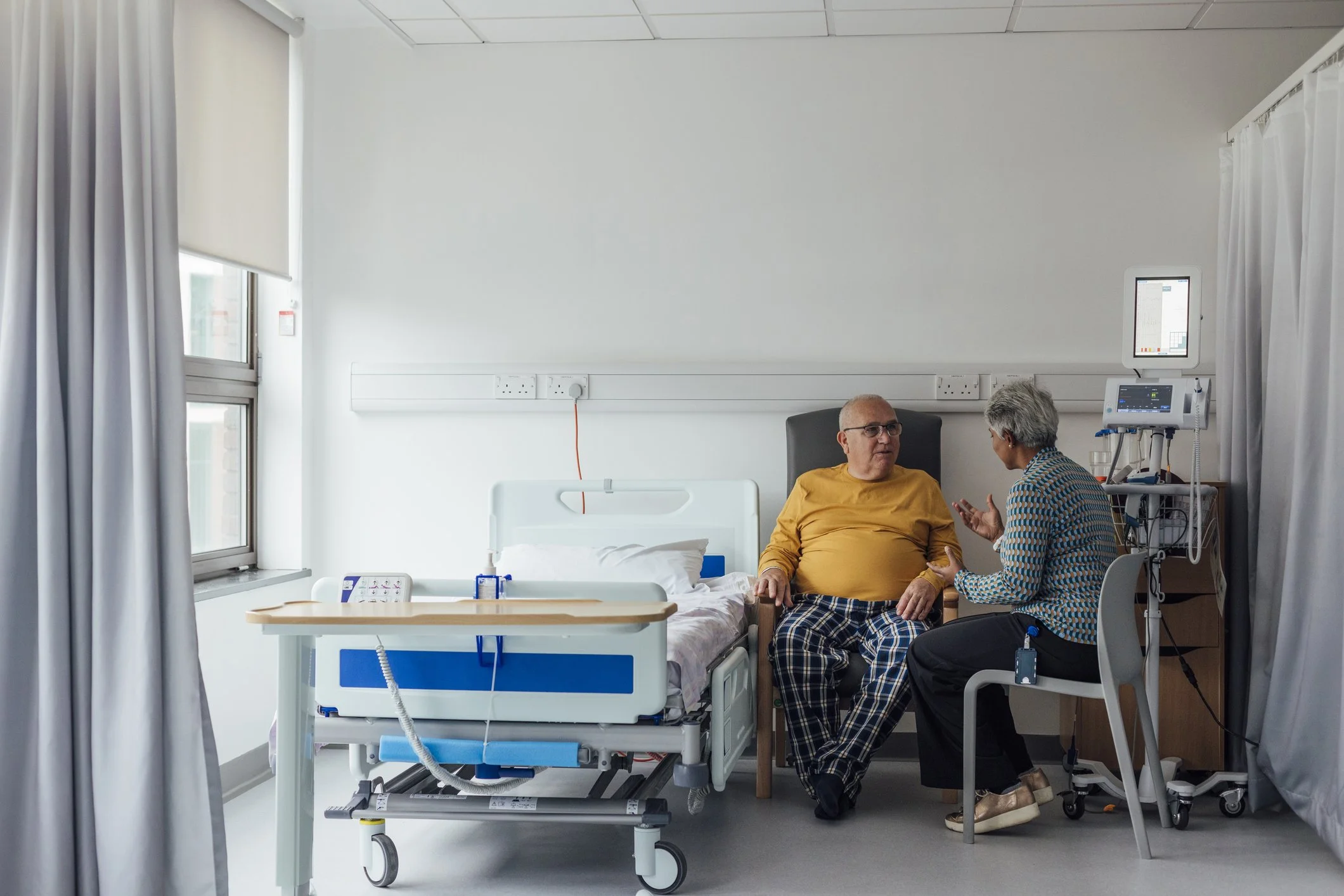
Cancer Surveillance and Age: When Risk, Benefit and Priorities Shift
Age changes the context of cancer care. This article explains how surveillance and treatment decisions evolve as risk, health and priorities shift over time.

Living With Cancer on Active Surveillance: Practical and Emotional Support
Living with cancer on active surveillance can feel harder than expected. This article explores the practical and emotional realities, and how patients are supported over time.
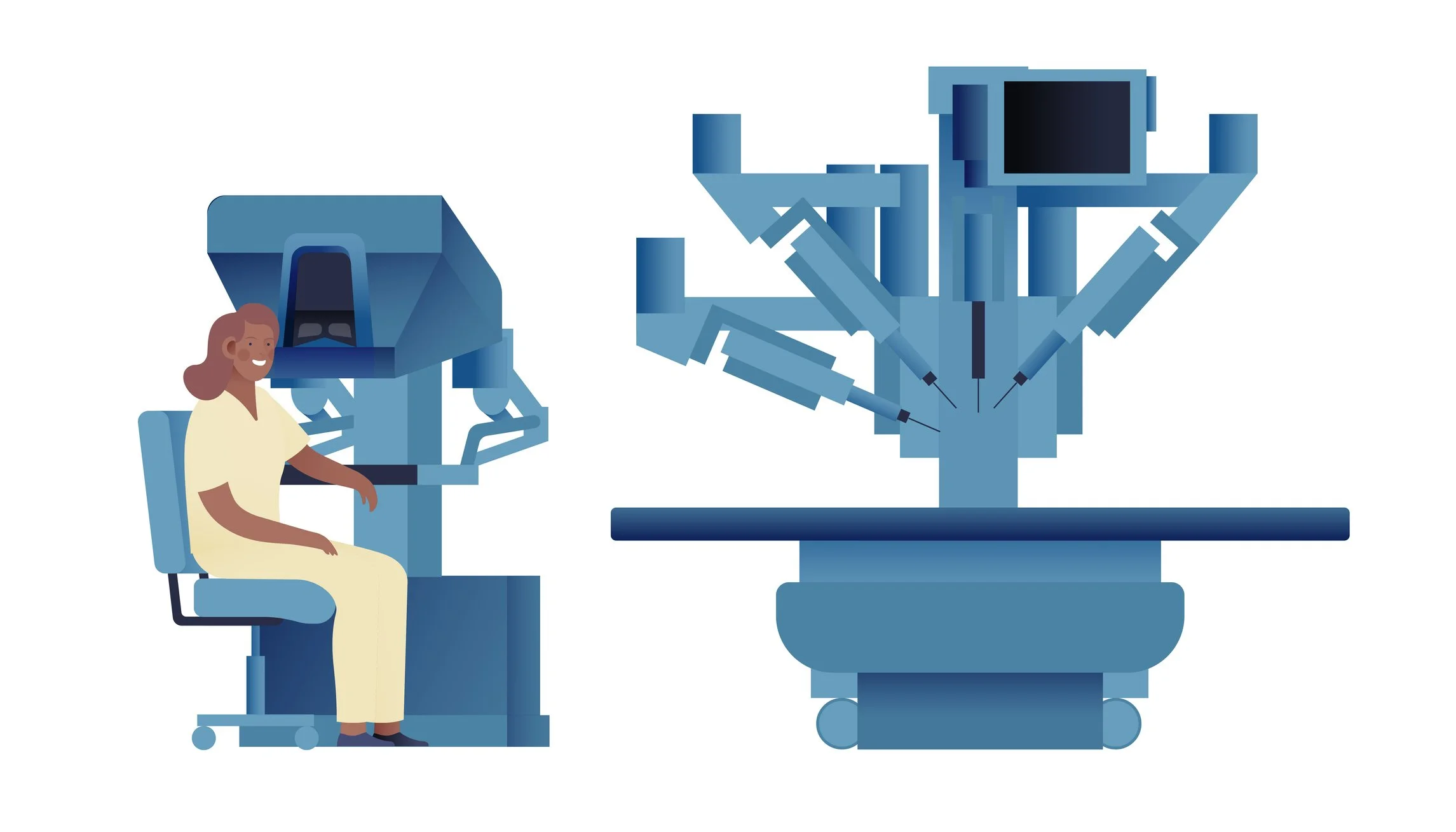
Robotic Surgery for Kidney Cancer: What the Robot Changes — and What It Doesn’t
Robotic surgery is a tool in kidney cancer care — not the treatment itself. This article explains when robotic surgery helps, when it doesn’t, and how decisions are really made.

Robotic vs Open Surgery in Urologic Cancer: What Changes, and What Doesn’t
Robotic surgery can reduce blood loss and shorten hospital stay for some urologic cancer operations—but it doesn’t guarantee better cancer control or functional outcomes. Here’s how the decision is actually made, and when open surgery remains the safer choice.

Life After Radical Cystectomy: What Patients and Families Should Expect
An honest overview of life after radical cystectomy, including recovery, urinary diversion, emotional adjustment and how patients and families adapt over time.
Active Surveillance in Urologic Cancer: When Doing Less Is the Right Decision
Active surveillance can be the right choice for selected urologic cancers. Learn when monitoring is appropriate, how risk is assessed, and what follow-up involves.

Recovery After Robotic Cancer Surgery: What Patients Underestimate
Recovery after robotic cancer surgery is rarely linear. This article explains what patients often underestimate about fatigue, function and emotional adjustment.
